The Changing Face of the Nursing and Residential Care Industry
June 21, 2024In the United States, there were 92,850 nursing and assisted living facilities (all ownerships) employing 3.3 million workers in 2023. The nation’s nursing and assisted living sector lost 400,893 employees from early 2020 (pre-pandemic) to the end of 2022, according to the Bureau of Labor Statistics. This amount of job loss in these industries far outpaced other health care sectors in the nation.
Broad Industry Definition
The residential care industry comprises establishments primarily engaged in providing residential and personal care for persons who choose to maintain their independence and do not need round-the-clock medical care. According to the National Institute on Aging, assisted living residents usually live in their own apartments and share common areas. They have access to many services such as three meals a day, assistance with personal care, housekeeping, and laundry.
Establishments in the nursing home industry are primarily engaged in providing inpatient nursing and rehabilitation services with the health services being largely some level of nursing services and round-the-clock medical care.
Oregon’s Nursing and Residential Care Industry
Oregon’s nursing and residential care industry (private ownerships) consisted of 1,997 facilities employing an average of 39,596 workers in 2023. This broad industry experienced a net loss of -3,833 jobs during the past two-year recessionary period but has now gained back these jobs and more.
Employment trends in Oregon’s assisted living facilities have not matched the employment trends in nursing homes. Since 2001, employment in assisted living consistently grew by an average of about 800 jobs a year until the pandemic hit in early 2020. Nursing homes, on the other hand, have experienced employment levels varying widely from year-to-year with 11 years of job losses from the period of 2002 through 2023.
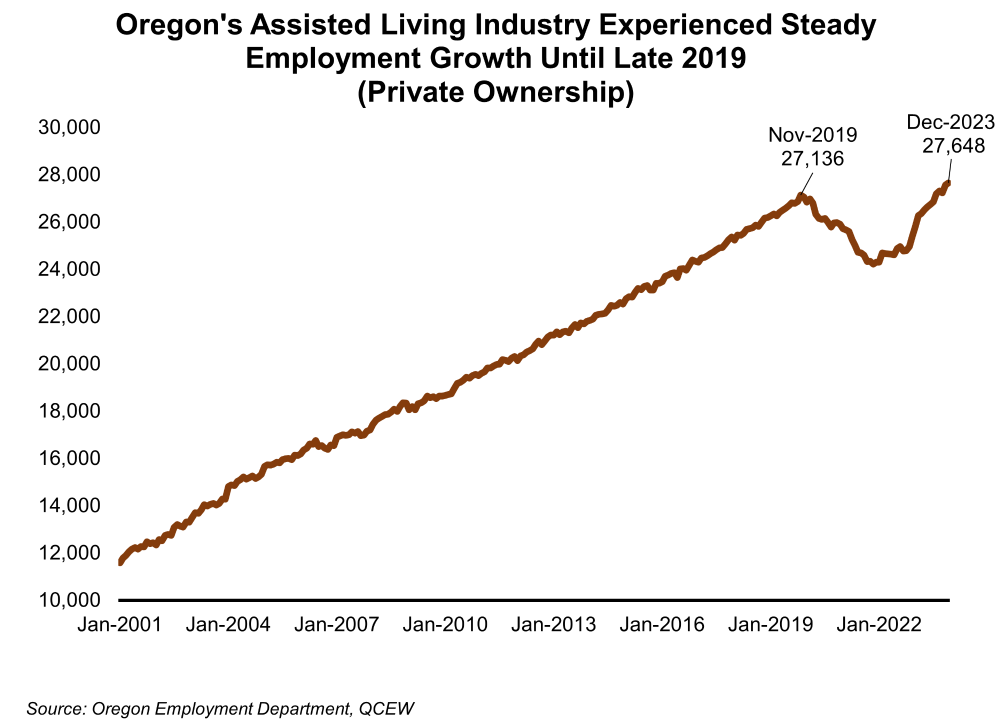
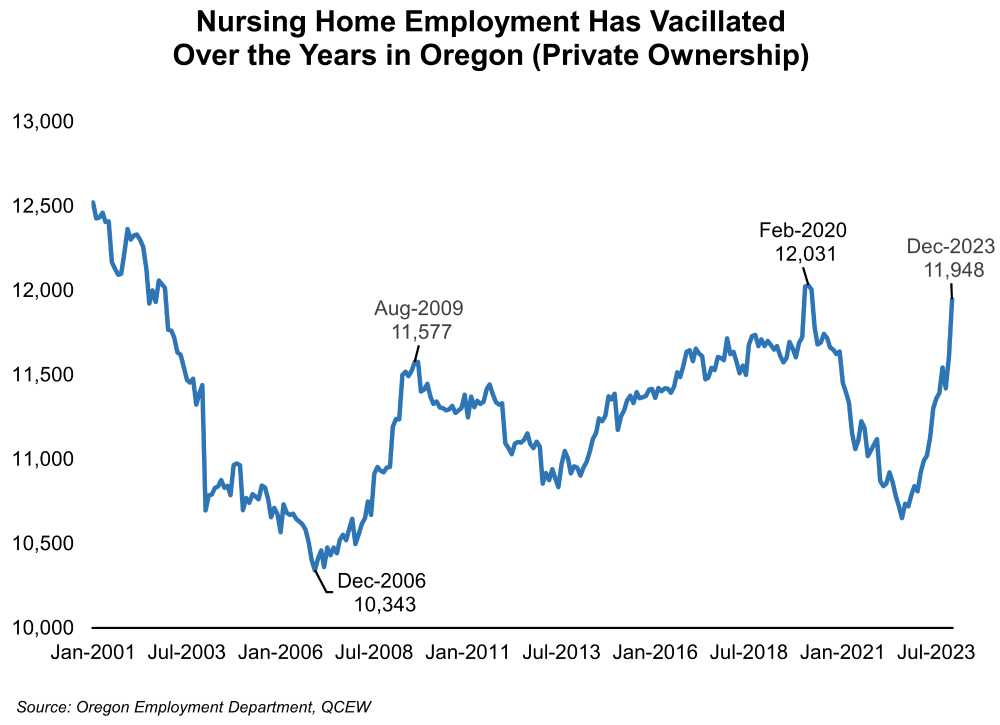
The number of assisted living facilities in Oregon outnumbered the number of nursing homes by nearly nine to one in 2023. Since 2001, the number of assisted living facilities have grown by 815 units, or by 72.5%, reaching 1,939 units in 2023. In contrast, the number of nursing home facilities has remained relatively stable, increasing by only 39 facilities, or by 19.8%, during the same period.
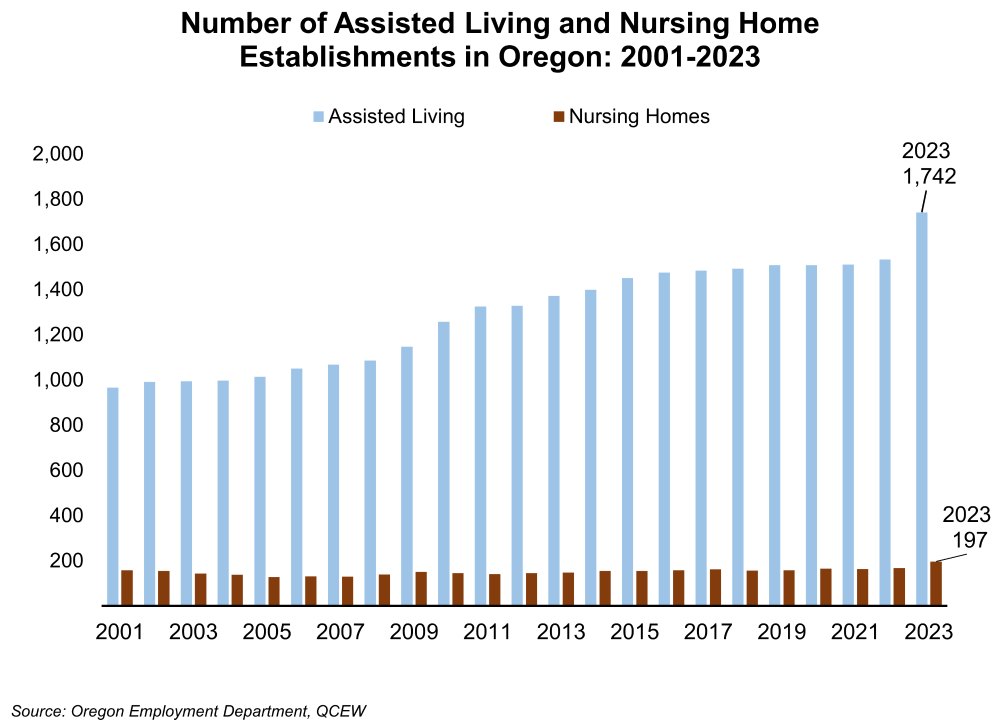
Demand for Long-Term Care in Oregon
Demand for long-term care options for seniors is expected to increase as Oregon’s older population continues to grow.
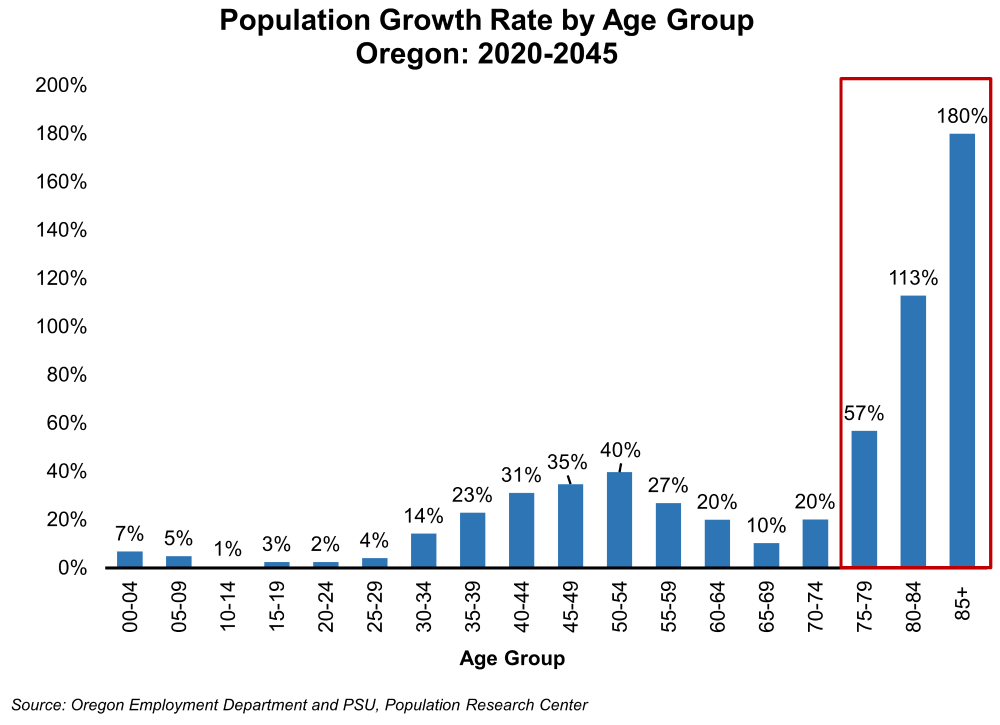
According to Portland State University’s Population Research Center, Oregon’s population 75 years and older is expected to increase by 344,312, or by 107%, from 2020 to 2045, reaching 664,980 by 2045. In stark contrast, the state’s population 24 years or younger is expected to grow by only 41,591, or by 3.3%, by 2045.
A similar picture emerges nationally, where the 65 and older population is projected to nearly double in size from 49 million in 2016 to 95 million in 2060. By 2060, the share of people aged 65 and older will compose nearly one-quarter of the population in the United States, according to the U.S. Census Bureau.
Who Works in Nursing and Residential Care Facilities?
The types of occupations in nursing home and residential care vary from health care services to food serving, grounds keeping, and building maintenance. Although varied, the majority of occupations (58%), or nearly 1.8 million workers, in the nation were in healthcare practitioner and healthcare support occupations in 2023. These specific occupations included nursing assistants, home health and personal care aides, licensed practical and vocational nurses, and registered nurses. The next largest occupations were in building cleaning, food serving, and housekeeping.
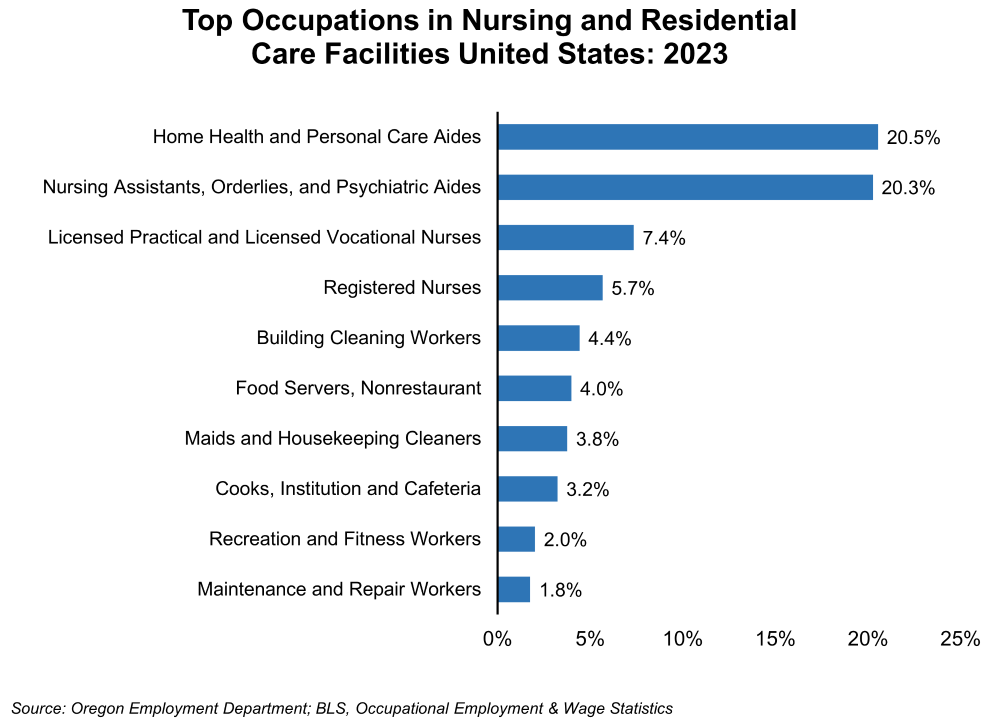
If we assume that Oregon has a similar occupational makeup as the industry does nationally, Oregon’s 2023 average hourly wage for the two largest occupations in long-term care would range from $17.93 for home health and personal care aides to $21.58 for nursing assistants, orderlies, and psychiatric aides, which are both healthcare support occupations. The average wage for all occupations in 2023 was $31.17.
The Cost of Long-Term Care Services
Genworth, a long-term care insurance company, has carried out an annual survey on the cost of long-term care since 2004. In Oregon, the monthly median cost of care was $5,825 in assisted living facilities and between $14,585-$15,208 in nursing homes. Nationally, the annual cost of care ran $64,200 for assisted living and $104,025-$116,8000 for nursing homes. According to Genworth, 10,000 baby boomers will turn 65 every day and seven out of 10 of these people will require long-term care services at some point in their lives until 2031.
The Industry Speaks Out: The State of Assisted Living and Nursing Homes in America
The American Health Care Association (AHCA) and the National Center for Assisted Living (NCAL) carry out a survey of nursing home and assisted living facilities each year. According to the AHCA and NCAL, the long-term care industry has been facing an unprecedented workforce challenge since the pandemic. A reported combination of workload, environment, low wages, reduced occupancy rates, and COVID-19 vaccine requirements have contributed to worker shortages. More than 300 nursing homes have already closed since the pandemic began.
The following includes the main conclusions from the June 2022 assisted living and nursing home surveys:
State of the Assisted Living Industry, June 2022
- More than one-half of assisted living facilities are experiencing a worse staffing situation since the beginning of 2022 with 63% of facilities facing moderate or high staffing shortages.
- 87% of assisted living communities are experiencing difficulty hiring staff and nearly all are asking staff to work more.
- Nearly one-third of facilities are either limiting new admissions or closing their facilities due to staffing shortages.
- Over 90% of facilities have increased staff wages but consider lack of interested or qualified candidates and the inability to offer competitive wages an obstacle to hiring new staff.
- Nearly 40% of facilities are operating at a loss and nearly one-half are concerned about having to close over staffing woes.
- Assisted living facilities estimate that their costs have increased by 40% in one year and one-third say they cannot sustain the current pace for more than one year.
State of the Nursing Home Industry, June 2022
- 60% of nursing homes are experiencing worse staffing shortages since the beginning of 2022 and 87% face moderate or high staffing shortages.
98% of nursing homes are experiencing difficulty hiring staff and 61% are limiting new admissions.
- While nine out of 10 nursing home providers have offered increased wages and bonuses, lack of either interest or qualified candidates are the top obstacles in hiring new staff.
- Nursing home providers estimate their costs have increased by 41% in one year and 73% of providers are concerned they may have to close due to staffing woes.
- Nearly 60% of nursing homes are operating at a loss and more than one-half report that they cannot sustain their current pace for more than one year.
- According to AHCA, women account for nearly 90% of nursing home and assisted living employees while also making up the majority of nursing home residents at nearly 70%.
The Changing Face of the Nursing and Residential Care Industry
The current workforce shortages in the long-term care industry, exacerbated by the pandemic, are causing some establishments to halt admissions or close completely. Many workers in this industry face low pay and poor working conditions, and long-term care facilities find it difficult to compete with other industries for workers. Meanwhile, the rapidly growing population of older adults is expected to drive demand for long-term care even higher in years ahead.
The pandemic has also sparked a national conversation about where and how people want to live as they age and need increasing assistance. A recent poll by The John A. Hartford Foundation found that 57% of older adults say that COVID-19 has affected their willingness to live in a nursing home and 89% say that changes are needed to make nursing homes more acceptable and inviting to them.
Alternatives to traditional nursing homes are becoming more popular which include programs like GRAYCE, which helps family caregivers support older adults, or The Greenhouse Project, which is a creation of non-institutional eldercare environments that resemble traditional homes.
Lastly, more and more health care services are now being carried out in an individual’s home, which can encourage more elders to “age in place”. Thanks to today’s technology, many elders can receive varied professional health care services in their homes, paid for by Medicare as if they were in a hospital. According to a recent article titled Providers Betting Big on Future of Hospital at Home, the American Hospital Association (AHA) explains that the hospital at home model has grown significantly since the Center for Medicare and Medicaid Services (CMS) launched its waiver program in 2020. According to AHA, in April 2024 CMS had authorized more than 320 hospitals in 37 states to offer acute hospital care at home. As technology advances, it seems reasonable that elders who are comfortable with technology like computers and cell phones will continue to demand home-based delivery of medical care and remote monitoring which could enable them to stay in their homes much longer than in prior years.